Maternity
Pregnancy is considered to last approximately 40 weeks (280 days) from the last menstrual period (LMP), or 38 weeks (266 days) from the date of conception. However, a pregnancy is considered to have reached term between 38 and 42 weeks. Babies born before the 37 week mark are considered premature, while babies born after the 42 week mark are considered postmature.
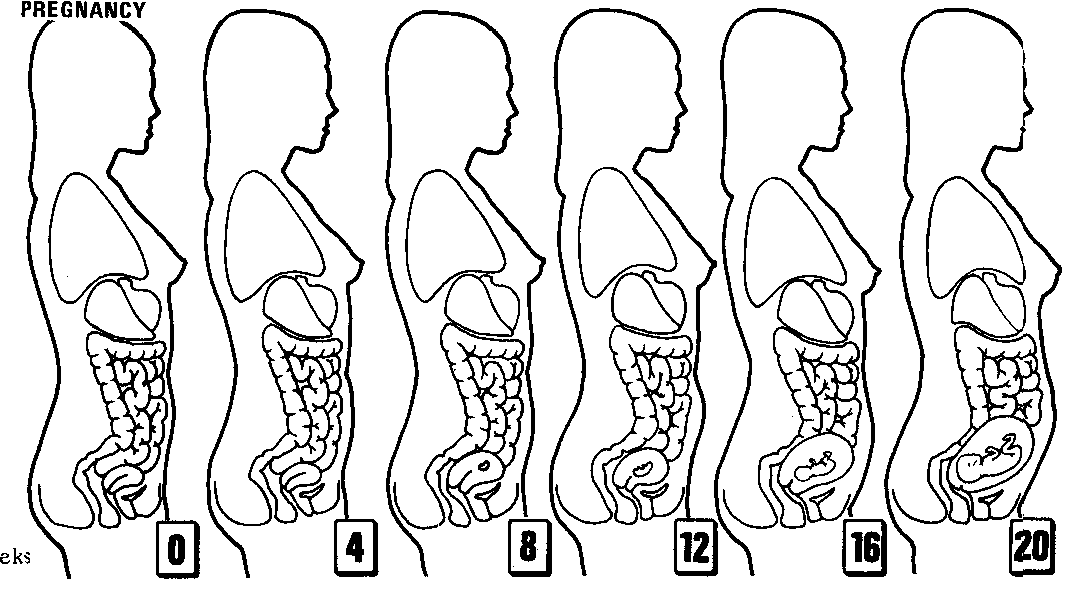
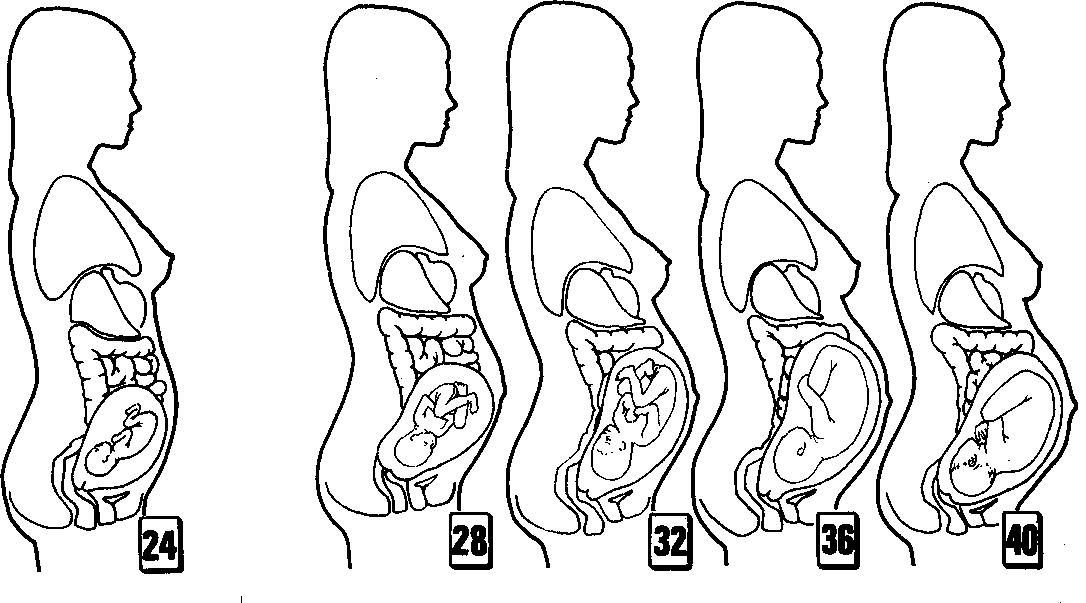
During pregnancy, the mother undergoes many physiologic changes, be they cardiovascular, renal, haematological, metabolic or respiratory, changes that become very important in the event of complications.
- Plasma and blood volume increase by 40-50% to accommodate
the changes
- Results in overall vasodilation, increased heart rate (15 bpm), stroke volume, and cardiac output
- Diastolic blood pressure consequently decreases between 12-26 weeks, and increases by 36 weeks. If the blood pressure remains abnormal beyond 36 weeks, the mother should be investigated for preeclampsia, a condition that precedes eclampsia.
- Pregnant women often have the sensation of shortness of breath
First Stage of Labour
- This phase can take typically 12-14 hours if this is the first pregnancy.
- Show - mucous discharge from the vagina, which may be tinged with blood. Anything more than a tinge of blood be sure to get patient to hospital ASAP
- Contractions - coming at regular intervals and the cervix begins to dilate. Patient contractions will then gradually become stronger and more frequent, and last longer. While the experience of labour can vary widely, a typical one might start out with contractions coming every ten minutes, lasting 30 seconds each, and gradually increasing to every five minutes, lasting 40 to 60 seconds each.
- "waters breaking " refers to the rupture of the membranes surrounding the baby and the gush or the leaking of amniotic fluid through the vagina.
View 1st Stage of Labour Diagram
Management
Encourage mother to adopt a comfortable position, Entonox for pain relief, Transport to hospital as this might be your only opportunity
Second Stage of Labour
The second stage of labour starts when the cervix is fully dilated and ends when the baby is born. If this is a second pregnancy then this process can be very quick.
- This stage lasts typically 60 minutes to 2 hours.
- Contractions during this stage may be several minutes apart.
- The woman will have a strong urge to push. (it's not unusual for the woman to have her bowels open during this stage - be prepared)
Management
- Contact control to ask for a midwife to attend,
- Prepare the stretcher with blankets and incontinence pads,
- Open maternity pack,
- Prepare warm blanket for the arrival of the baby,
- Reassure mother,
- Continue to offer pain relief,
- Patient comfort in a semi recumbent position,
- If enroute to hospital safely pull over and stop the ambulance.
N.B - Try to consider modesty with certain ethnic minorities. It could be extremely worrying for a women to be attended by a male crew. Try to minimise this anxiety and if possible allow a female member of staff to deal with the patient.
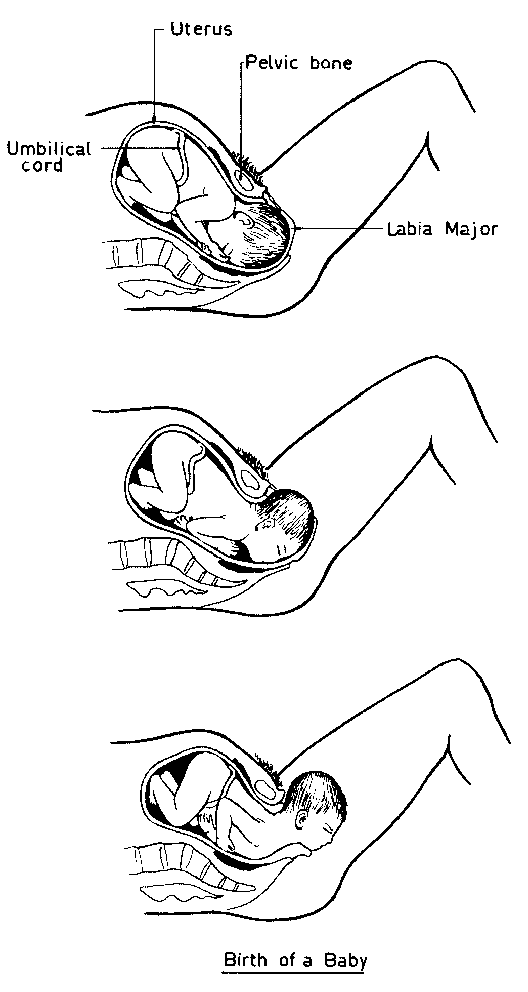
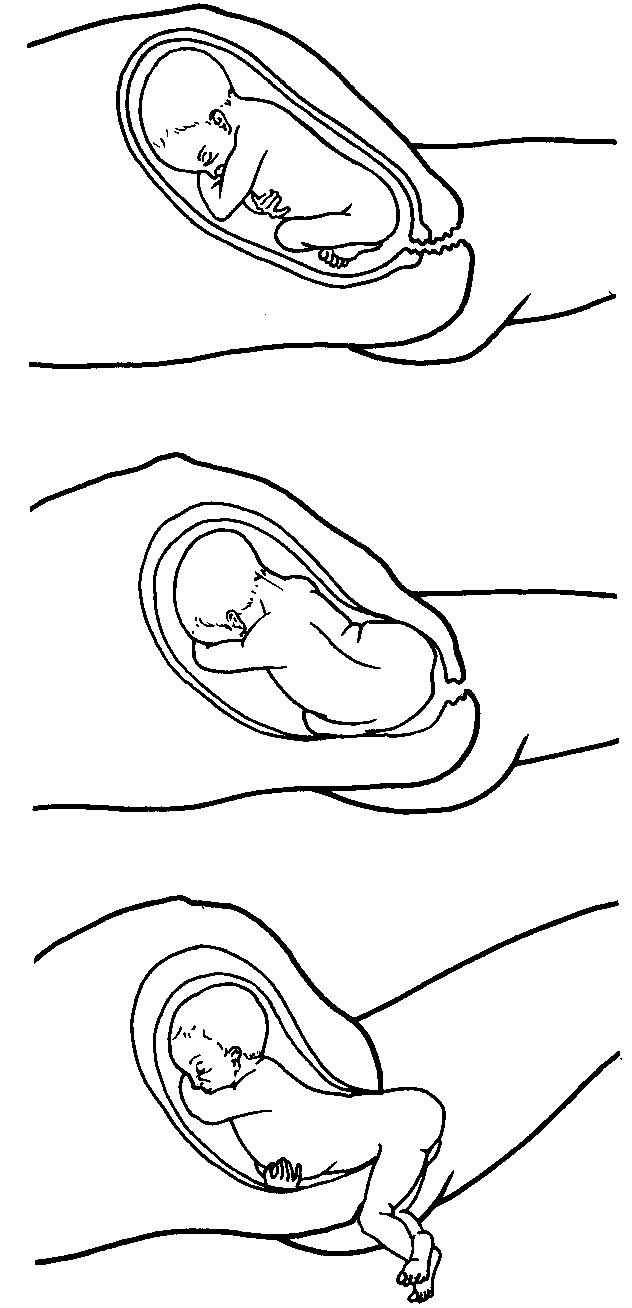
Delivery of the Baby
Click here to view stages of delivery
- Remind mother to try to pant, or only push very gently with the contractions.
- As the baby's head becomes visible, place your hand on the head and provide it with support to keep it from popping out (Do not apply pressure though). Getting mother to pant during this part will help prevent tearing of the perineum. (If tearing occurs and has not stopped after baby is born apply a pressure dressing)
- After the baby's head is completely out, dry her off with a clean towel and wipe her nose and mouth to clear away any mucus and blood.
- If necessary clear her airway with a mucus extractor, but only the oral cavity.
- If the rest of the body has not yet made its way out, her head should then be guided gently downward toward the floor to deliver the top shoulder. Then, to deliver her bottom shoulder, gently lift her body toward the ceiling.
- Once the shoulders are delivered, the rest of the body will be born fairly quickly. It is very important to be aware that the baby will be extremely slippery, so use extra caution in holding her.
- If the baby is not breathing or crying at this point, stimulate her to take her first breaths by firmly rubbing her back or by gently slapping the soles of her feet. Drying her off with a towel also can stimulate her and will prevent her from getting cold.
- If she is cyanosed then enrich the atmosphere with oxygen
- If the baby continues to not breathe, she may require rescue breathing.
- Dry off the baby as much as possible with clean, dry towels. Once she is dry, place her skin-to-skin on her mother's abdomen so that she can benefit from her mother's body heat. Cover mother and baby with a warm blanket
- Apply two cord clamps securely about 6 inches from the umbilicus and cut the cord between the clamps( Only if accepted by local protocols)
- If local protocols don't allow cord cutting, then if the cord is long enough, encourage the new mother to breastfeed her baby if she is willing. This will trigger additional uterine contractions, which will help to expel the placenta and reduce postpartum bleeding.
- Once the placenta is expelled, which can take anywhere from a few minutes to a half hour, it should be placed next to the newborn. You still do not want to cut the cord.
Third Stage of Labour
After the baby is born, the mother will continue to have contractions, but they will not be as uncomfortable as the contractions she experienced while she was in labour. The placenta will separate from the wall of the uterus. As this occurs, she may feel an urge to push as the placenta makes it's way into the birth canal, and the placenta will be delivered. Place the placenta into a bowl so that staff at the hospital can check it is intact. After the placenta has been delivered the mother may bleed a little but this should not be anymore than 200 - 300 mls. If the bleeding doesn't seem to be easing then gentle massage on the abdomen just above the umbilicus will start uterine contractions and the bleeding should begin to decrease.
Management
- Do not pull on the cord but to allow natural delivery of placenta
- Deliver into a bowl for hospital staff to inspect
- Massage abdomen at point of umbilicus. As you massage the uterus should start to harden and begin to ease bleeding.
- NOTE: If the placenta has not been delivered by 30 mins of the baby arriving it is classed as the placenta being in retention. Also if the placenta partially separates, potential life threatening haemorrhage could occur
Childbirth Complications
- Cord Prolapse: when the umbilical cord precedes the fetus' exit from the uterus it is said to be 'prolapsed' Although the baby does not have to be visible from the entrance of the vagina. It is an obstetric emergency during pregnancy or labour that imminently endangers the life of the fetus. Cord prolapse is rare and has an annual incidence of 0.1 - 0.6%, however this number increases to 1% in breech births.
- Shoulder dystocia: after the delivery of the head, the anterior shoulder of the baby cannot pass below the pubic bone. It is diagnosed when the shoulders fail to deliver shortly after the head. During delivery it is said the baby shows the 'turtle neck sign', which involves the appearance and retraction of the fetal head as the chin presses against the walls of the perineum.
- Breech Presentation: In the breech presentation the baby enters the birth canal with the buttocks or feet first as opposed to the normal head down presentation. Again incidences are low at around 3-4% in woman who are 'Term' however 1 in 5 pregnancies are breech at 28 weeks gestation.
There are 3 common breech presentations:
- Frank 65% - Bottom first with legs flexed at hips and legs extended from the knees.
- Complete 25% - Hips and knees are flexed as if the foetus is crossed legged.
- Footling 10% - One or both feet come out first. Very rare but more common in premature births.
Management of Cord Prolapse
- Now's not the time to be embarrassed: you will need to 'expose and visually examine' the patients genital area
- This is TIME Critical. This, as an out of hospital emergency, throws challenges at 'us' as the attending crews. If birth is not imminent it's "how do we transport this woman to hospital?" Ideally having the patient in a head down on her knees with them pulled into her chest is great. This position allows gravity to act on the foetus and prevents further possible compression of the cord. But this position will not be safe to transport the patient.
- When you have the patient next to the trolley get her to lay on her left side (avoid her sitting on her bottom as this may further complicate cord compression). Once in a left lateral position you'll need to raise her hips with blankets or lifting the foot end of the trolley.
- Once the cord is presenting outside of the vagina it is susceptible to the cooling and drying effects of the outside world and thus provoking spasm which will ultimately cut off blood flow. So with only one attempt (keep handling to a minimum) the cord needs to be replaced into the vagina using two fingers. If this is successful apply a dry pad to the entrance of the vagina to reduce the risk of another prolapse. Depending on which literature you read or your own trust protocols, it is also said that once the cord has been inserted into the vagina then the attendant should keep their fingers inserted in the vagina until the patient has been taken to the appropriate obstetric facility.
- It may not be possible to insert the cord back into the vagina. If this is the case moisten a piece of gauze with WARM normal saline will need to be applied to the cord, keeping handling to a minimum, and try to keep Warm and MOIST during transit
ASHICE (Consider)
Transport to Hospital
Professional Handover
Management of Shoulder Dystocia
- Once again another TIME Critical emergency
- If, while attempting normal delivery, the baby's head does not seem to be progressing beyond the perinium ensure you immediately update control that you may be dealing with shoulder dystocia so that the attending midwife can be informed
- UNDER CONSTRUCTION
ASHICE (Consider)
Transport to Hospital
Professional Handover
Management of Breech Presentation
Under Construction