Patient Assessment
Below are the stages you take from the moment you arrive at the scene of an incident to when you safely get your patient to the appropriate receiving hospital
Survey of the Scene/Approach
- Gloves on
- Danger
- Scene History (What has happened, get info visually and Verbally)
- Patient level of consciousness on the AVPU scale
Primary Survey
- Airway - Clear. Aspirate if necessary
- C-Spine - Consider spinal immobilisation if an injury is suspected
- Breathing - Head tilt, chin lift, Jaw thrust. Look, Listen and Feel. Consider adjuncts to maintain airway. Oropharyngeal or Nasopharyngeal. If no respiratory effort use a Bag and Mask with 100% O2 if available.
- Circulation - Feel for a carotid pulse. If no pulse
consider Precordial thump. Recheck pulse if absent commence
chest compressions. Control any
Major Bleeding
Secondary Survey
- History taking - Asking questions about signs and symptoms i.e.. When did they start etc. Previous Medical History
- Conduct a Top to Toe examination
- Record pulse and respiratory rates
Patient Management/Transport
- T.L.C
- Appropriate Care for Patient's Particular Complaint
- Smooth journey to hospital
Continually Reassess Patient
- Carry on monitoring for any changes in condition
- Carry out thorough observations e.g. BP, ECG, SPO2 etc
Pre-Alert Call to Receiving Hospital
- A - Age
- S - Sex
- H - History of event
- I - Injuries sustained
- C - Condition of patient. GCS, Revised Trauma Score, BP etc
- E - Estimated Time of Arrival at Hospital
Patient History
Obtaining an accurate account is a critical first step in determining the history of a patient's chief complaint. History taking is an 'art' in itself and will take a little while to get to grips with, on top of thinking what could be wrong and what treatment you should give. This is the time when your crewmate will be able to help you out when your thoughts go blank. More often than not asking just one question will put you back on track.
Some points to taking a patient history:
- Introduce yourself to the patient. Add a smile as this will help put them at ease
- If possible bring yourself to their level and not talk down to them
- Ask them their name. Older people often like to be addressed by their surname, but ask which name they'd like to be known as.
- Try not to be too informal by using names like sweetheart, darling, love.
- Ask open ended questions to start with. Something like "What's been happening today" or "What made you call for an ambulance"
- Try and get the patient to be specific as to why the ambulance has been called, this may require you to push for the chief complaint as patients can wander off track and drift back 10 years to when they had flu if you not careful.
- A patient may have a number of complaints that they may want to talk about. You can only deal with one at a time so each condition will have to be explored individually
Follow up questions such as those below will be the next step in gaining a successful history. As an example I will use the types of questions asked of a patient with a complaint of pain.
A simple phrase to make remembering the types of questions easier - OPQRST
- O - Onset (Did problem develop suddenly or gradually? What was patient doing when pain came on?)
- P - Provocation (What provokes the pain? What palliates the pain?)
- Q - Quality (What the pain feels like, stabbing, dull,sharp, burning or crushing? Try to allow the patient to describe the pain as they may tell you what they think you want to hear, and note this on your report form)
- R - Radiation/Region (Where is the pain? Does the pain stay in one place or is the pain felt anywhere else? If the pain radiates, where does it radiate to?)
- S - Severity (Score pain from 1 to 10 or in case of children use the Wong-Baker FACES pain scale. Are there any associated symptoms = e.g., nausea, vomiting, dizziness?)
- T - Time (How long has pain been present? Is it constant of does it come and go? How long has it been affecting your patient (Chronic or Acute))
Neurological Assessment
The Glasgow Coma Scale is a simple but effective way of assessing a patients neurological condition. It categorises the patients responses to certain stimuli and gives that response a score. It is divided into 3 main categories of response.
Best Motor
Response
6 Obeys Commands
5 Localises pain.
4 Withdrawal to pain
3 Flexion
2 Extension
1 No response to pain.
Best Verbal Response
5 Oriented
4 Confused conversation
3 Inappropriate words
2 Incomprehensible sounds
1 No verbal response.
Eye Opening
4 Spontaneous.
3 Open to speech
2 Open to pain.
1 No eye opening.
Pulse
Definition of a Pulse: The throbbing of a person's arteries as an effect of their heart beat, which can be felt at the wrist and other places
Pulses are manually palpated with two fingers, generally the pointer and middle finger. The thumb must not be used because it has its own pulse that will be felt instead of the patient's pulse. The two fingers must be placed near to an artery in order to feel the blood pulsating through the circulatory system.
Major Pulse Points
- Radial pulse - located on the thumb side of the wrist
- Carotid pulse - located in the neck
- Brachial pulse - located in between the bicep and tricep; frequently used in place of carotid pulse in infants, who have no neck
- Femoral pulse - located in the thigh
- Dorsalis pedis pulse - located on top of the foot
Taking a pulse is a good indicator as to whether a PT's heart rate is fast (Tachycardia), Slow (Bradycardia), whether the PT has a Regular or Irregular beat and if the pulse is Strong or Weak. A pulse is also felt for in the case of a fracture to see whether or not blood is flowing to the distal point of a limb past the site of injury. The palpability of a pulse is dictated by the patient's blood pressure (See topic below for info on Blood Pressure).
Other types of assessment that are carried out while performing your secondary survey
Auscultation - The technical term for listening to the internal sounds of the body, usually using a stethoscope. Auscultation is normally performed for the purposes of examining the cardiovascular system and respiratory systems (heart and lung sounds), as well as the gastrointestinal system (bowel sounds).
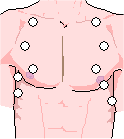
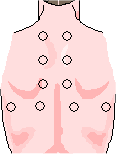
Approximate Auscultation Sites
-
Auscultate from side to side and top to bottom
-
Avoid the area over the scapulae
-
Note any differences in sounds from each side
-
List findings on Patient Report Form
Palpation - a method of examination in which you feel the size, shape or firmness of body parts. Palpation is used particularly for thoracic and abdominal examinations, but also for examination and palpation of pulses.
Percussion - is a method used to find out about the changes in the thorax or abdomen. It is done with the middle finger of one hand tapping on the middle finger of the other hand, which is positioned with the whole palm on the body. Depending on what is happening in the structure below, this will create a different type of sound. e.g. If a patient has a pneumothorax, when you tap on the affected side it will sound like you are tapping on a drum compared to the non affected side.

Pulse and Respiratory Rates (These figures vary depending on the literature you read)
|
Respirations |
|
|
Descriptors: Normal, Shallow, Laboured, Noisy, Kussmaul |
|
|
Adult >12years (normal) |
12 to 20 (breaths/min) |
|
Age 2 - 12 years |
20 - 30 (breaths/min) |
|
Age 1 - 2 years |
26 - 34 (breaths/min) |
|
<1 Year |
30 - 40 (breaths/min) |
|
Pulse |
|
|
Descriptors: Regular, Irregular, Strong or Weak |
|
|
Adult |
60 to 100 beats per minute |
|
Children - age 1 to 8 years |
80 to 100 |
|
Infants - age 1 to 12 months |
100 to 120 |
|
Neonates - age 1 to 28 days |
120 to 160 |
Blood Pressure
Blood pressure is the name given to the force that the beating heart causes in the arteries, veins, and blood vessels which carry blood around the body. When the heart contracts, forcing blood through the arteries and other blood vessels, your blood pressure goes up, and falls when the heart relaxes. High blood pressure can cause heart problems and strokes.
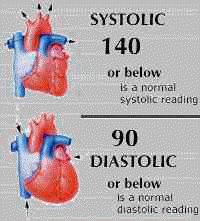
When blood pressure is measured, the result is given as two figures, one higher than the other, for example 120/80. This is because tests measure the pressure in vessels when the heart is contracting (the higher figure also called systolic blood pressure), and then when it is relaxing (the lower figure also called diastolic blood pressure).
How to measure blood pressure
 Blood pressure is measured using a cuff which is placed around the upper arm and inflated until tight. It then deflates and
a blood pressure reading is taken.
Blood pressure is measured using a cuff which is placed around the upper arm and inflated until tight. It then deflates and
a blood pressure reading is taken.
The target for adults is for blood pressure to be below 140/90, or below 130/80 in people with diabetes. It is advised that if blood pressure is above this range, action should be taken to bring it down.
Why high blood pressure is a concern
If blood pressure is high it causes a strain on blood vessels and the heart. High blood pressure can also cause kidney problems, and heart failure, when the heart is unable to pump blood around the body properly.
The higher the blood pressure is, the greater the risk of stroke, heart problems and kidney failure.
Causes of high blood pressure
People with a family history of high blood pressure, stroke, or heart disease are more likely to have high blood pressure. Diabetes and kidney disease also increase the risk.
Blood pressure can be raised by diet and lifestyle. Being overweight increases blood pressure, as does eating a fatty diet and drinking too much alcohol. Smokers, people who consume too much salt, and those who do not take regular vigorous exercise are also more likely to have high blood pressure.
How to take a manual Blood Pressure
Tools required: sphygmomanometer and a stethoscope
The following steps may be helpful to take a blood pressure.
- Sit up or lie down with the arm stretched out. The arm should be level with the heart.
- Put the cuff about 1 inch (2.5 cm) above the elbow (over the brachial artery). Wrap the cuff snugly around the arm. The blood pressure reading may not be correct if the cuff is too loose.
- Put the stethoscope earpieces in your ears.
- Using your middle and index fingers, gently feel for the brachial pulse. You will feel the pulse beating when you find it.
- Put the diaphragm of the stethoscope over the brachial artery pulse. Listen for the heartbeat.
- Tighten the screw on the bulb and quickly squeeze and pump the bulb. This will cause the cuff to tighten.
- Keep squeezing the bulb until the scale on the gauge reads about 160. Or, until the gauge reads at least 10 points higher than when you last hear the heartbeat.
- Slowly loosen the screw to let air escape from the cuff. Carefully look at the gauge and listen to the sounds. Remember the number on the gauge where you first heard the thumping sound.
- Continue to listen and read the gauge at the point where the sound stops.
- The number of the first sound is the systolic (top number) pressure.
- The second number is the diastolic (bottom number) pressure.
Estimating Blood Pressure
The advanced trauma life support course teaches that a patients systolic blood pressure can be "estimated" if you haven't got a sphygmomanometer to hand. This is achieved by feeling for a pulse, i.e.
- If a Radial pulse is present then the PT's systolic BP is > 80mmHg
- If a Brachial pulse is present then the PT's systolic BP is 70-80mmHg
- If a Carotid pulse is present then the PT's systolic BP is 60-70mmHg
This is only a rough guide and should not replace taking a proper blood pressure reading as soon as possible.